What is Lyme disease?
Lyme disease, also known as Lyme borreliosis, is a bacterial infectious disease caused by bacteria of the Borrelia genus — spirochaetes, or spiral-shaped bacteria. In humans, the infection is most commonly transmitted through the bite of an infected tick. The disease can affect the skin, nervous system, joints and, more rarely, the heart.
The Latvian Centre for Disease Prevention and Control (SPKC) describes Lyme borreliosis as an infection that can affect several organ systems and usually involves damage to the skin, nervous system, heart and joints.
Several Borrelia species occur in Europe, so the manifestations of Lyme disease may differ — in one patient, the disease may mainly present with skin redness, while in another it may involve the nervous system, joints or general symptoms.
It is important to understand:
- not every tick bite causes infection;
- not every tick carries Borrelia bacteria;
- the bite of an infected tick does not automatically mean that a person will become ill;
- Lyme disease recognised in time is treatable in most cases.
Lyme disease is not the same as tick-borne encephalitis. Lyme disease is caused by bacteria, while tick-borne encephalitis is caused by a virus. This difference is important because Lyme disease is treated with antibacterial therapy prescribed by a doctor, whereas vaccination is available against tick-borne encephalitis.
Main signs that may indicate Lyme disease
Lyme disease should be considered especially if one or more of the following signs appear after a tick bite or after staying in an area where contact with ticks is possible:
- a gradually expanding area of redness on the skin, especially if it is at least 5 cm in diameter;
- flu-like symptoms — fatigue, fever, chills, headache;
- muscle or joint pain without another clear cause;
- facial nerve weakness or asymmetry, numbness, tingling;
- recurrent or migrating joint pain, especially in the large joints.
The U.S. Centers for Disease Control and Prevention state that early symptoms usually appear within 3–30 days after a tick bite, while erythema migrans gradually expands and may reach a large diameter.
Where is Lyme disease common?
Lyme disease is one of the most common tick-borne infections in Europe and North America. In Latvia, it is a practically significant infection because ticks are found not only in forests and meadows, but also in parks, gardens and suburban areas. SPKC states that a person may become infected with Lyme disease after the attachment of an infected tick.
The risk is not limited to “deep forest”. Ticks may also be found:
- in household lawns;
- in parks;
- in berry-picking and mushroom-picking areas;
- near bodies of water;
- in places with tall grass, bushes and leaf litter.
Incidence statistics in Latvia
In Latvia, Lyme disease is one of the most significant tick-borne infections. Statistics published by SPKC show that the number of Lyme disease cases varies from year to year: for example, during the period from 2017 to 2025, between 272 and 612 cases were registered annually, while in 2025 there were 539 cases.
These data should be interpreted as a general trend, because incidence is influenced by tick activity, weather conditions, people’s time spent outdoors, diagnostic frequency and reporting practices. Current data on Lyme disease and other tick-borne diseases are available on the SPKC website.
Who is at risk?
People who frequently spend time in environments where ticks are present have an increased risk of Lyme disease.
Risk groups:
- people who go to forests, meadows or shrubland;
- mushroom pickers, berry pickers, hunters and anglers;
- gardeners and residents of rural areas;
- children who play in grass or parks;
- people who work outdoors — in forestry, agriculture or territory maintenance;
- pet owners, because animals can bring ticks into the home;
- people who do not check their body and clothing after spending time outdoors.
The level of risk increases if the tick is not noticed and remains attached for a long time.
Mechanism of infection
Lyme disease develops when an infected tick attaches to human skin and Borrelia bacteria enter the body during the bite.
In simplified terms, the mechanism of infection is as follows: during its life, a tick may become infected by feeding on the blood of an infected animal. Later, when it attaches to a human, it may transmit the bacteria further.
Borrelia bacteria do not always enter the body immediately at the moment of the bite. SPKC explains that, unlike the tick-borne encephalitis virus, which may enter the bloodstream more quickly, borrelia may enter the body from the tick later, and the risk of infection increases if the tick has remained attached for longer.
Lyme disease is usually not transmitted:
- from person to person;
- through touch;
- through coughing or sneezing;
- through food;
- through everyday household contact.
Timeline of infection and symptom development
The diagram below helps to understand how Lyme disease may develop after a tick bite. This is a general timeline — symptoms may differ for each patient.
Tick bite — the moment of possible infection, when Borrelia bacteria may enter the body.
The first hours or days after the bite — the tick should be removed as soon as possible. A small local redness or irritation may appear at the bite site, which is often non-specific and may go unnoticed.
Within 3–30 days after the bite — the characteristic erythema migrans may develop — a gradually expanding red patch, often with a lighter centre. Flu-like symptoms may also occur, such as fatigue, fever, headache, as well as muscle and joint pain.
Within weeks to months — if the infection spreads in the body, systemic symptoms may appear: nervous system disorders, joint pain, skin changes, and more rarely carditis, meaning inflammation of heart structures, with subsequent rhythm disturbances.
Months later or later — if the disease is not recognised and treated in time, it may progress to a late stage, presenting with chronic joint inflammation, persistent fatigue and neurological complaints.
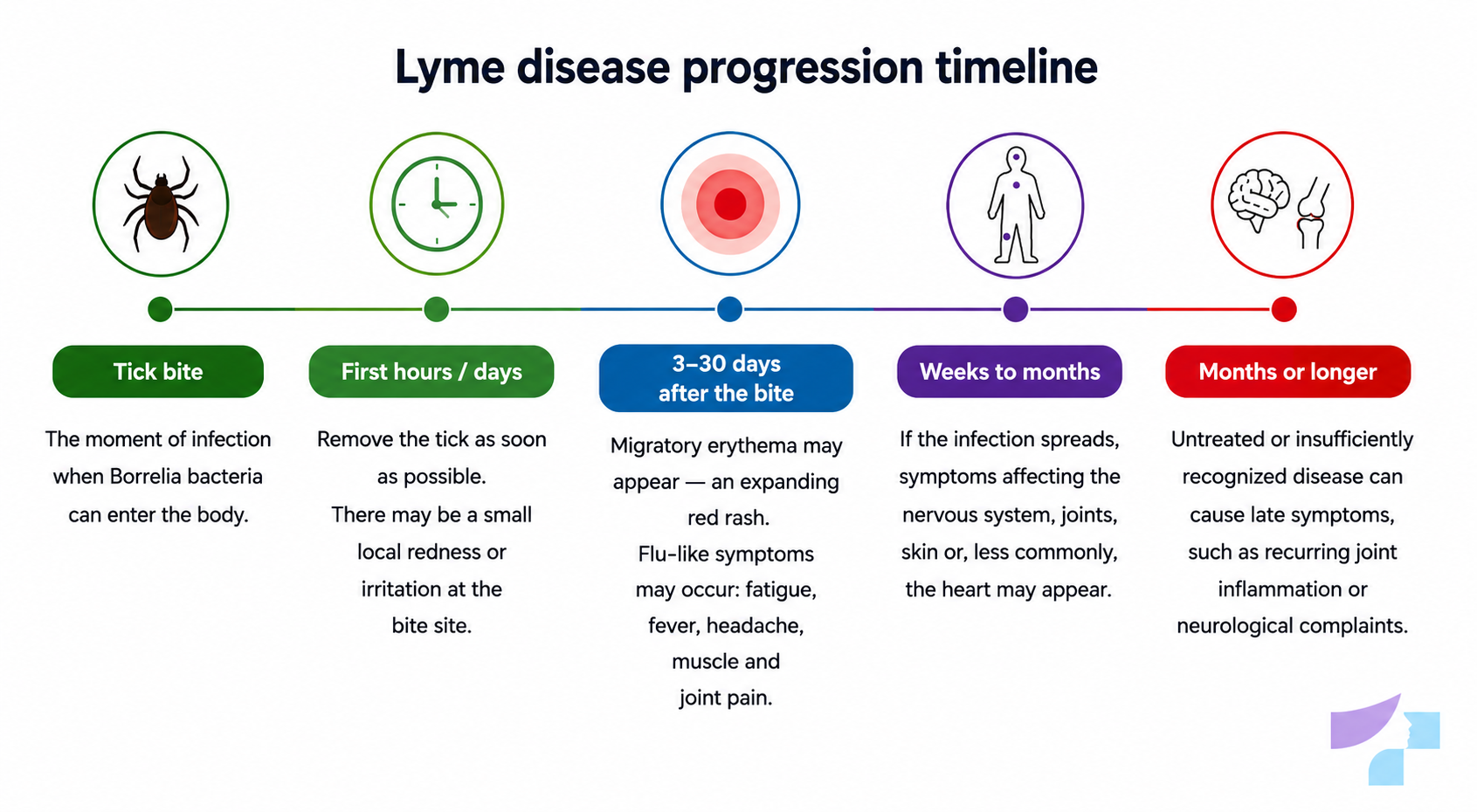
SPKC states that the most common symptom of Lyme borreliosis is erythema migrans — skin redness that appears at the site of tick attachment after 1–4 weeks. The U.S. Centers for Disease Control and Prevention describe the early symptom window as 3–30 days after a tick bite.
Early symptoms of Lyme disease
Early Lyme disease often begins several days to a few weeks after a tick bite. A person does not always notice the bite, because the tick may be very small and the bite is usually painless.
Typical early signs:
- fatigue;
- elevated temperature;
- chills;
- headache;
- muscle pain;
- joint pain;
- enlarged lymph nodes;
- general malaise;
- an expanding reddened patch on the skin.
In some patients, early symptoms may be mild, non-specific or resemble a viral infection. This is one of the reasons why Lyme disease is sometimes not recognised immediately.
What does a Lyme disease rash look like?
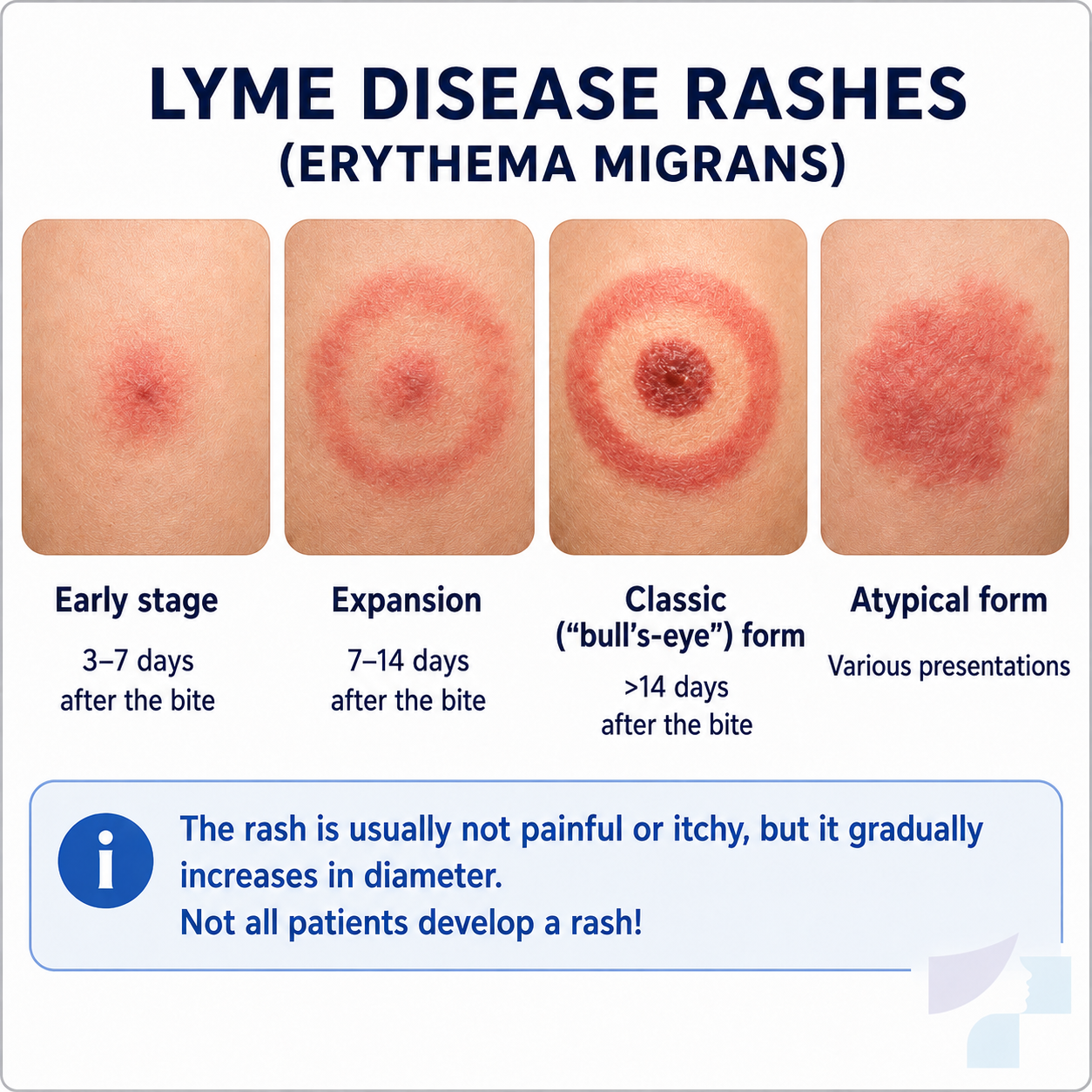
The most characteristic skin symptom of Lyme disease is erythema migrans — an expanding area of redness that usually appears at the bite site. It may be the classic “target” or ring-shaped rash, but it does not always look exactly like this.
A Lyme disease patch may be:
- round or oval;
- uniformly red;
- with a lighter centre;
- target-shaped or ring-shaped;
- warm to the touch;
- usually not particularly painful and not always itchy;
- gradually increasing in diameter.
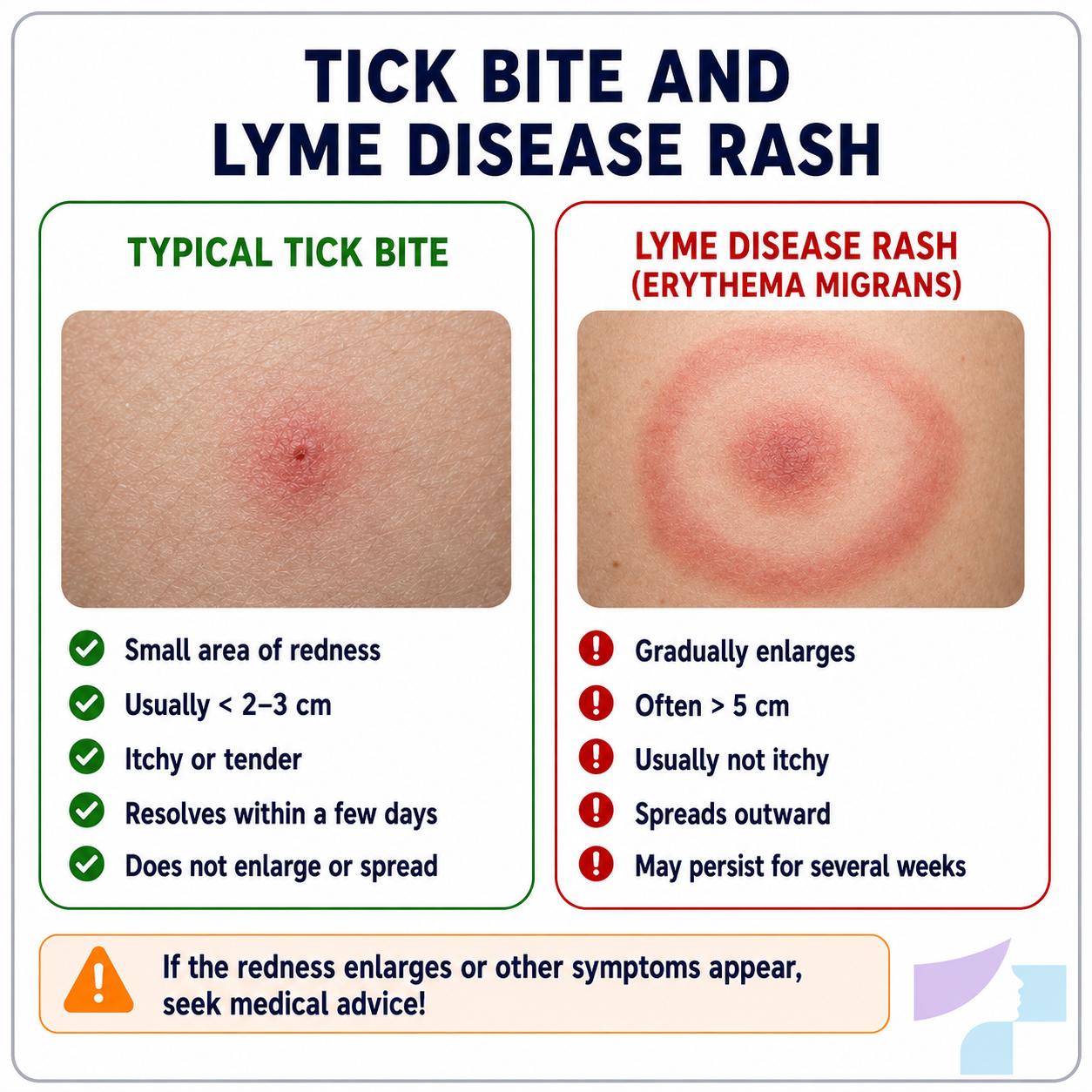
Important: a small area of redness immediately after a tick bite is not the same as erythema migrans. Local skin irritation is usually smaller and does not expand. A Lyme disease rash typically enlarges. The U.S. Centers for Disease Control and Prevention state that erythema migrans rashes often expand over several days and may reach a large size.
Symptoms
Early symptoms
In the early stage, Lyme disease most often presents with skin changes and general symptoms of infection.
Early symptoms may include:
- erythema migrans;
- fatigue;
- fever;
- chills;
- headache;
- muscle pain;
- joint pain;
- enlarged lymph nodes;
- feeling unwell.
Not all patients have the classic rash. Some may have only non-specific symptoms, so the doctor evaluates not only laboratory tests, but also the patient’s history, the possibility of a tick bite and the clinical picture.
Late symptoms
If Lyme disease is not recognised and treated, the infection may spread beyond the initial bite site. SPKC states that, more rarely, symptoms may appear indicating involvement of the nervous system, joints and, in some cases, the heart.
Late symptoms may include:
- recurrent or long-term joint inflammation;
- swelling of large joints, especially the knees;
- nerve pain;
- tingling or sensory disturbances;
- facial nerve damage;
- meningitis-like symptoms;
- memory or concentration difficulties;
- heart rhythm or conduction disorders;
- marked fatigue.
These symptoms are not specific only to Lyme disease. They may also be signs of other diseases, so medical evaluation is necessary.
Typical symptom combinations
Lyme disease can present in different ways. In practice, it is important to recognise symptom combinations that, together with the possibility of a tick bite, increase suspicion of the disease.
Expanding skin patch and fatigue
This is a classic combination of early Lyme disease. If the patch is enlarging and appeared days or weeks after a tick bite, medical consultation is necessary.
Fever, headache and muscle pain after being outdoors
This picture may resemble a viral infection, but if contact with ticks was possible, tick-borne infections should also be considered.
Joint pain and previous skin redness
If joint pain or swelling appears later after a previous rash, medical evaluation is necessary.
Facial nerve weakness and headache or neck stiffness
This combination may indicate involvement of the nervous system, including neuroborreliosis.
Palpitations or faintness and a recent possibility of Lyme disease
In rare cases, Lyme disease may affect the heart, so such symptoms should be taken seriously.
Stages of Lyme disease
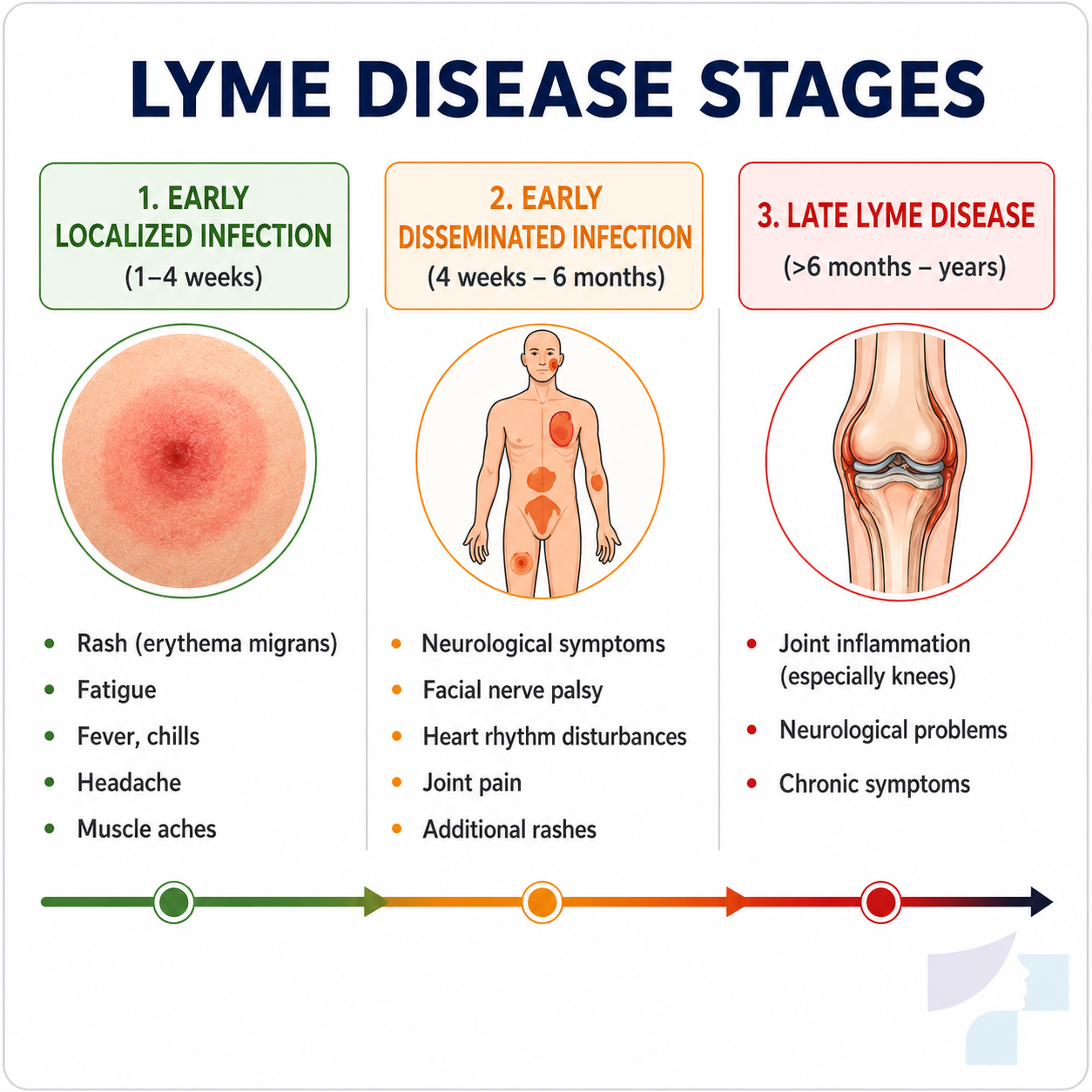
Early localised infection
At this stage, the infection is mainly associated with the bite site.
Typical signs:
- erythema migrans;
- fatigue;
- mild fever;
- headache;
- muscle or joint pain.
At this stage, treatment is usually most effective.
Early disseminated infection
Disseminated infection means that the bacteria may have spread further in the body. The nervous system, joints, skin or, more rarely, the heart may be involved.
Possible manifestations:
- multiple areas of skin redness;
- facial nerve paralysis;
- nerve pain;
- meningitis-like symptoms;
- migrating joint pain;
- more rarely carditis, meaning inflammation of heart structures, with subsequent rhythm disturbances.
Late Lyme disease
Late Lyme disease may appear months or longer after an untreated infection.
Possible manifestations:
- recurrent joint inflammation;
- persistent joint pain;
- neurological symptoms;
- peripheral nerve damage;
- cognitive complaints, such as difficulty concentrating.
What is neuroborreliosis?
Neuroborreliosis is a form of Lyme disease involving the nervous system.
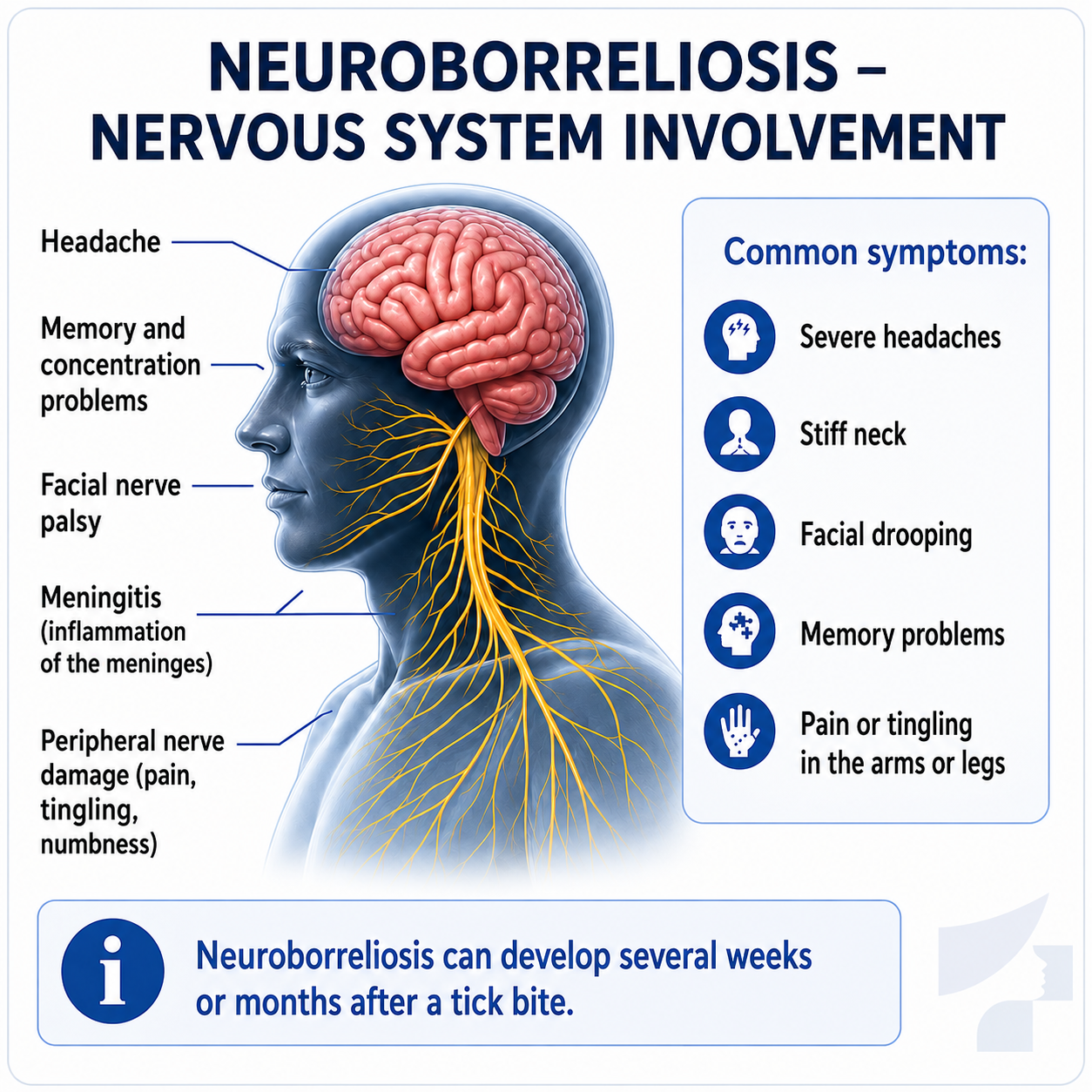
It may present with:
- nerve pain;
- tingling;
- sensory disturbances;
- facial nerve damage;
- headache;
- meningitis-like symptoms;
- concentration or memory difficulties.
Neuroborreliosis is a medically serious condition that must be evaluated by a doctor. Self-diagnosis in this situation is not safe.
Can Lyme disease affect the heart?
Yes, but this happens less often. Lyme disease may cause cardiac conduction disorders, meaning a situation in which electrical impulses in the heart are conducted incorrectly.
This may present with:
- palpitations;
- dizziness;
- weakness;
- a feeling of faintness;
- shortness of breath;
- unusual fatigue.
If heart symptoms appear after a tick bite or Lyme disease symptoms, urgent medical consultation is necessary.
Consequences and complications
Lyme disease treated in time ends in recovery in most cases. The greatest risks arise when the disease is not recognised or treatment is delayed.
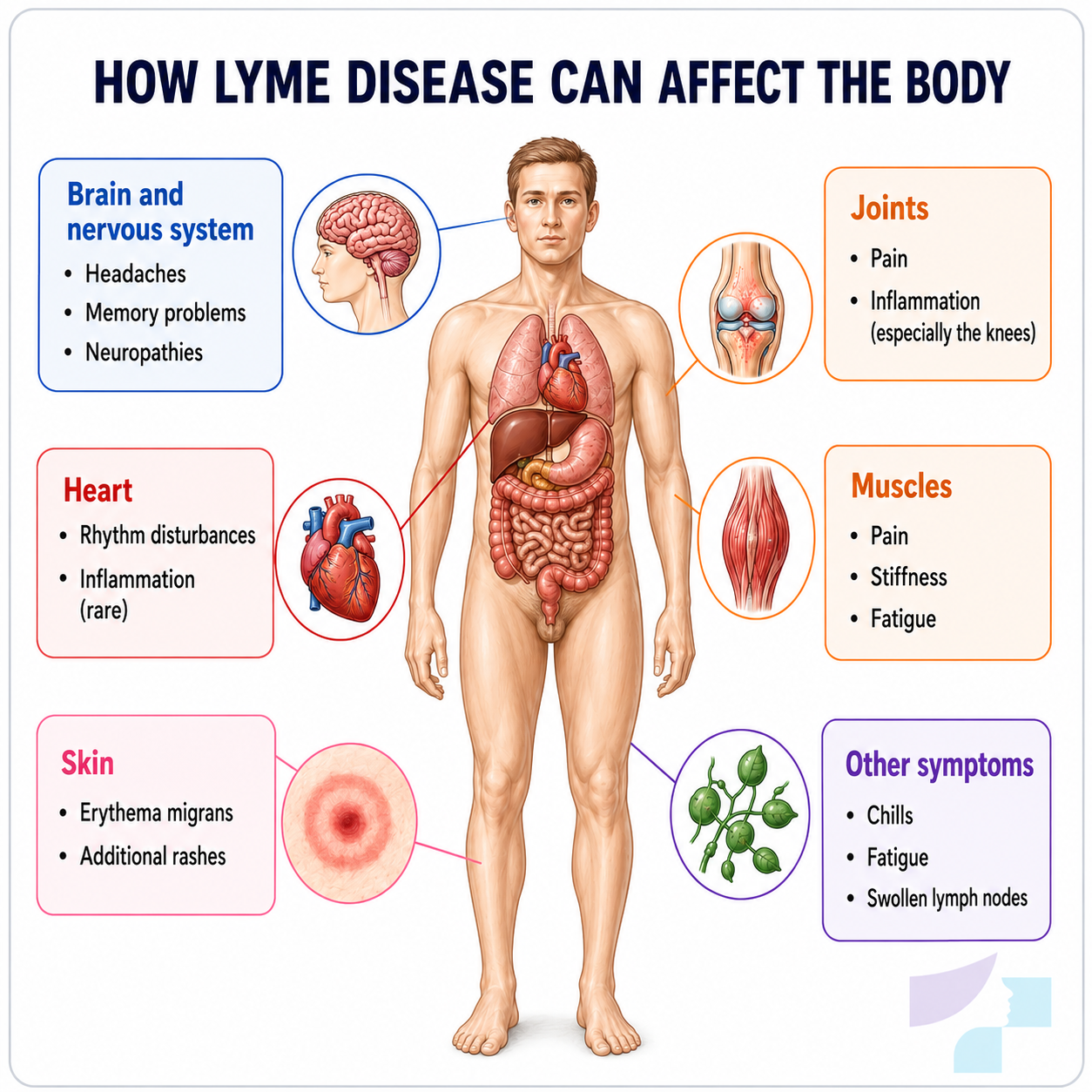
Possible consequences:
- long-term joint pain;
- recurrent joint inflammation;
- nervous system damage;
- sensory disturbances;
- facial nerve paralysis;
- heart rhythm or conduction disorders;
- persistent fatigue;
- cognitive complaints.
It should be emphasised that these symptoms may also occur in other diseases. Therefore, differential diagnosis is important — the doctor’s process of distinguishing between possible diseases.
How is Lyme disease diagnosed?
The diagnosis of Lyme disease is based on a combination of several factors.
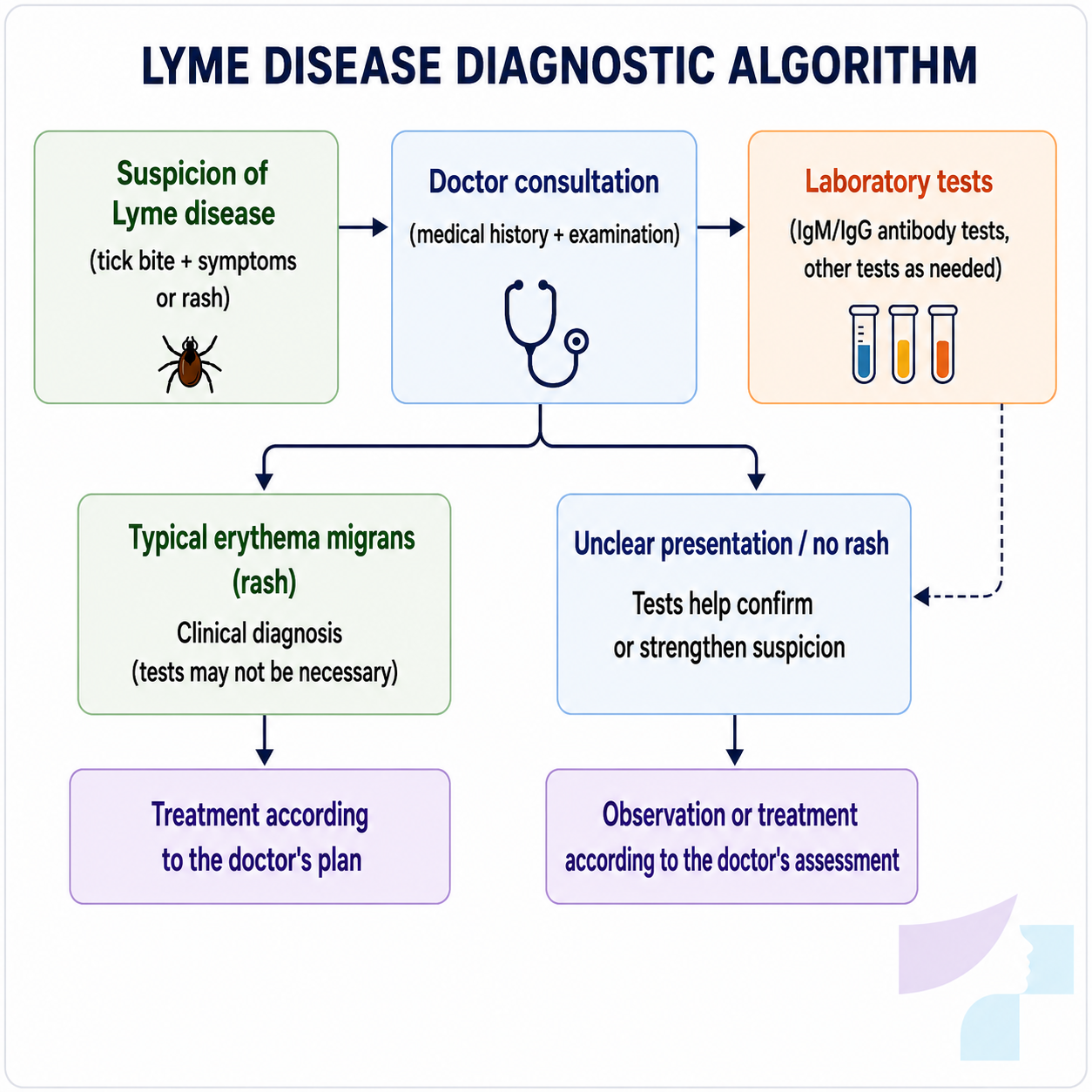
Medical history
The doctor evaluates:
- whether there has been a tick bite;
- whether the patient has stayed in a place where contact with ticks was possible;
- when the symptoms appeared;
- how the symptoms changed over time;
- whether there was characteristic skin redness.
Clinical picture
Typical erythema migrans is a sufficiently significant sign for diagnosis. In the early stage, laboratory tests will not always be positive immediately.
Laboratory tests
Antibody tests may be used, for example:
- IgM antibodies;
- IgG antibodies.
Important: positive antibodies do not always mean active disease, because they may persist after a previous infection. Conversely, in the early stage of the disease, antibodies may not yet have developed, so the test may be negative. Therefore, test results must always be interpreted together with symptoms and a doctor’s evaluation.
Can Lyme disease be completely cured?
In most cases — yes. Lyme disease recognised early usually responds well to antibacterial therapy prescribed by a doctor. The earlier treatment is started, the lower the risk of complications.
Can Lyme disease be treated without antibiotics?
In evidence-based medicine, the treatment of Lyme disease is based on antibacterial therapy prescribed by a doctor. Self-treatment, food supplements or unproven alternative methods must not replace treatment prescribed by a doctor.
This article does not specify particular prescription medicines or doses, because the choice of therapy is determined by the doctor, taking into account the patient’s age, symptoms, stage of disease, pregnancy, comorbidities and other factors.
What is “chronic Lyme disease”?
The term “chronic Lyme disease” is controversial and is used with caution in medicine. It is important to distinguish between several different situations:
- documented late Lyme disease;
- symptoms that persist after a treated infection;
- symptoms of other diseases that are mistakenly explained by Lyme disease;
- positive antibodies without evidence of active infection.
Is immunity possible?
After having Lyme disease, the body may develop an immune response — antibodies against Borrelia bacteria. However, this does not mean reliable and long-lasting protection against reinfection.
Reinfection is possible because:
- Borrelia bacteria have several species and variants;
- antibodies may persist, but they do not always provide complete protection;
- a new attachment of an infected tick may cause a new infection;
- positive antibodies alone do not prove active disease.
Therefore, a person who has once had Lyme disease should still follow tick-bite prevention measures.
What is Lyme disease often confused with?
Symptoms of Lyme disease may resemble many other diseases. Therefore, the diagnosis should not be made only based on a list of symptoms read online.
In differential diagnosis, the doctor may consider:
- viral infections;
- tick-borne encephalitis;
- rheumatological diseases;
- autoimmune diseases;
- symptoms of multiple sclerosis;
- chronic fatigue syndrome;
- neuropathies;
- other skin diseases;
- causes of heart rhythm disorders;
- other infectious diseases.
Lyme disease or tick-borne encephalitis?
| Feature | Lyme disease | Tick-borne encephalitis |
|---|---|---|
| Cause | Bacterium | Virus |
| Transmission | Tick bite | Tick bite |
| Basis of treatment | Antibacterial therapy prescribed by a doctor | Symptomatic and supportive treatment |
| Vaccination | No widely used routine vaccine | Vaccine available |
| Characteristic skin patch | Common | Not characteristic |
| Nervous system involvement | May occur | May be significant |
These diseases may begin after a tick bite, but they are not the same. The cause, prevention and treatment differ.
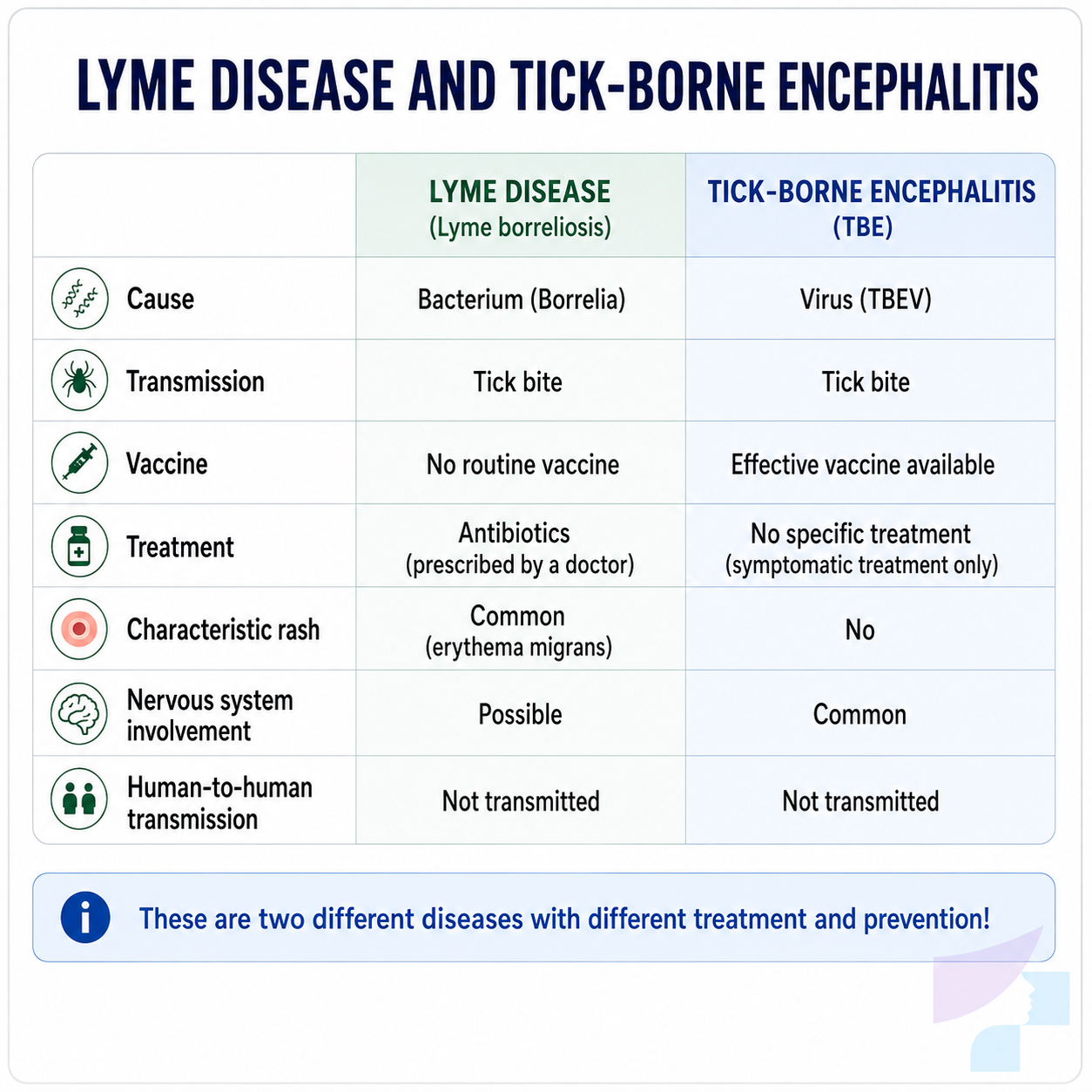
What happens if Lyme disease is not treated?
Untreated Lyme disease may spread in the body and cause more serious manifestations.
Possible consequences:
- joint inflammation;
- long-term joint pain;
- nervous system complications;
- facial nerve damage;
- sensory disturbances;
- more rarely, heart conduction disorders;
- persistent deterioration in general well-being.
This can be called the “cost of delay” — timely medical consultation is usually simpler, safer and less expensive than the diagnosis and treatment of delayed complications.
Lyme disease and pregnancy
If Lyme disease is suspected during pregnancy, a doctor should be consulted immediately. During pregnancy, treatment may only be chosen by a doctor, taking into account the safety of both the mother and the foetus. Self-treatment is not acceptable.
Prevention after a tick bite
How to remove a tick correctly?
Basic principles:
- the tick should be removed as soon as possible;
- an appropriate tool should be used — for example, fine-tipped tweezers or a tick-removal tool;
- the tick should be grasped as close to the skin as possible;
- it should be pulled steadily, without squeezing the tick’s body;
- the bite site should then be disinfected;
- health should be monitored over the following weeks.
You should not:
- apply oil to the tick;
- heat the tick;
- squeeze the tick’s body;
- wait for the tick to fall off by itself.

When should you see a doctor?
Medical consultation is necessary if, after a tick bite or possible contact with ticks, the following appear:
- expanding skin redness;
- fever;
- headache;
- marked fatigue;
- muscle or joint pain;
- facial asymmetry;
- tingling or numbness;
- palpitations, dizziness or faintness.

Preventive antibacterial therapy should not be started independently. In specific situations, it can only be assessed by a doctor.
Innovations and areas medicine is working on
Lyme disease remains an actively researched area of infectious diseases. In medicine, particular attention is paid to:
- more accurate early diagnosis;
- tests that better distinguish active infection from previous infection;
- biomarkers, meaning objectively measurable indicators;
- mechanisms of persistent symptoms after treated infection;
- vaccine development and effectiveness studies;
- better differentiation of patient groups to avoid both insufficient and excessive treatment.
The most important principle currently remains unchanged: timely recognition, medical evaluation and evidence-based treatment.
Conclusion
Lyme disease is a serious but, in most cases, treatable infection. The greatest risk is often not the tick bite itself, but delayed recognition of symptoms or attempts to interpret test results without a doctor’s help.
If expanding skin redness, flu-like symptoms, joint pain, nervous system symptoms or unexplained deterioration in well-being appear after a tick bite or time spent outdoors, a doctor should be consulted.
Important medical disclaimer
This material is for informational purposes only and does not replace medical consultation, diagnosis or treatment. The information is intended for patient education. If you have symptoms, suspected Lyme disease, worsening health or unclear test results, contact the clinic specialists listed below the article or another qualified healthcare professional. Do not attempt to diagnose yourself, interpret tests or start self-treatment without evaluation by a medical specialist.
References and authoritative sources
- Centre for Disease Prevention and Control (SPKC): Lyme borreliosis
- SPKC information material on Lyme disease
- SPKC: information on tick activity and Lyme disease transmission
- CDC: Signs and Symptoms of Untreated Lyme Disease
- CDC: Lyme Disease Rashes
- CDC: Lyme Disease overview
Content author
Dermatologist Dr. med. Dace Buile
